Pulmonary Function Test vs Chest X-Ray: What Is the Difference and Which One Do You Need?
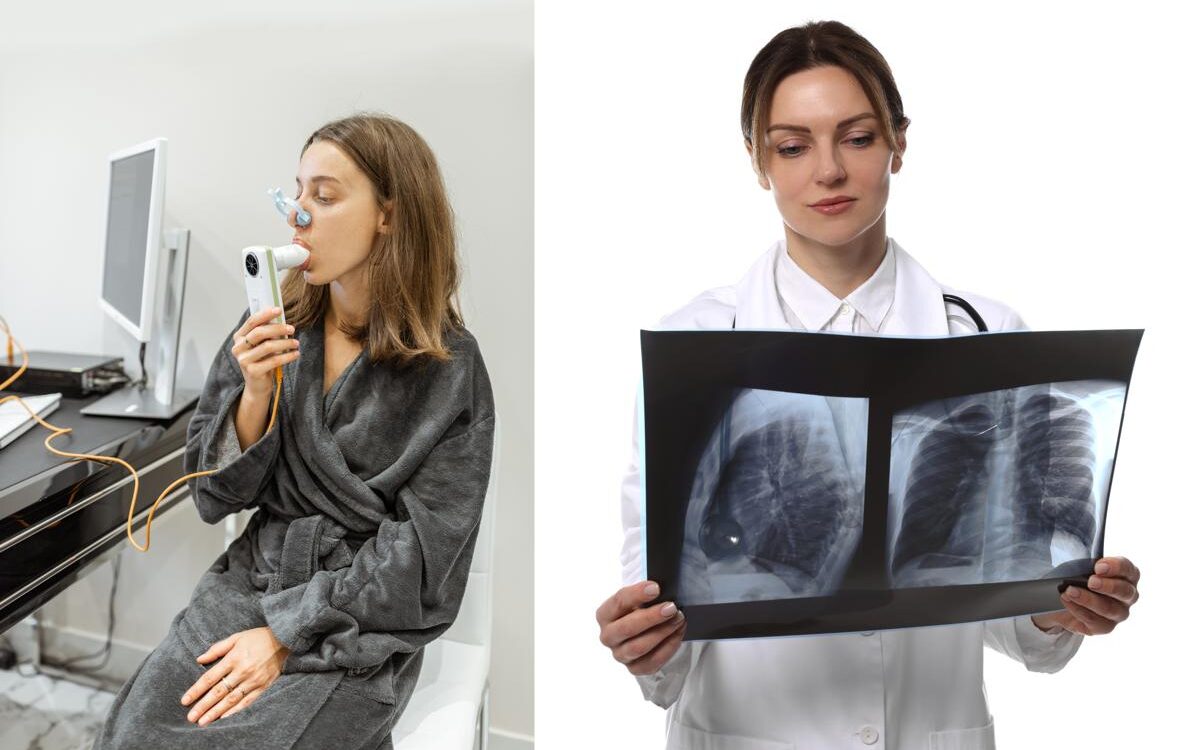
Pulmonary Function Test vs Chest X-Ray: What Is the Difference and Which One Do You Need? If your doctor has recommended lung testing, you may be wondering what the difference is between a pulmonary function test vs chest x-ray and which one is actually right for your situation. Both are used to evaluate respiratory health, but they measure completely different things, detect different conditions, and serve different clinical purposes. Knowing the difference helps you understand what your provider is looking for and why one test may be recommended over the other, or why both might be needed at the same time. This blog explains what each test does, what it can and cannot detect, how they compare directly, and which situations call for which approach. If you want a deeper look at how a PFT works on its own before reading the comparison, our guide on what a pulmonary function test is and what it measures is a helpful starting point. What Is a Pulmonary Function Test? A pulmonary function test, commonly called a PFT, is a non-invasive breathing test that measures how well your lungs work. Rather than producing an image of the lungs, a PFT measures the functional performance of your respiratory system, how much air you can inhale and exhale, how fast you can move air in and out, and how efficiently your lungs transfer oxygen into the bloodstream. The most common component of a pulmonary function test is spirometry, which measures: Forced vital capacity (FVC) – the total amount of air you can exhale after a full breath Forced expiratory volume in one second (FEV1) – how much air you can push out in the first second of exhalation The FEV1/FVC ratio – a key indicator used to identify airflow obstruction Additional PFT measurements may include lung volume testing, which assesses total lung capacity and residual volume, and diffusion capacity testing, which evaluates how efficiently oxygen crosses from the air sacs in the lungs into the bloodstream. According to the American Thoracic Society, pulmonary function testing is the standard diagnostic tool for detecting, classifying, and monitoring obstructive and restrictive lung diseases including asthma, COPD, and occupational lung conditions. A pulmonary function test is effort-dependent, meaning the accuracy of results depends on the patient breathing as hard and as fully as possible during the test. A trained technician guides you through the process to ensure results are reliable. What Is a Chest X-Ray? A chest x-ray is a form of medical imaging that produces a two-dimensional picture of the structures inside the chest, including the lungs, heart, ribs, and major blood vessels. Unlike a pulmonary function test, a chest x-ray does not measure how the lungs perform. It shows what the lungs look like structurally. A chest x-ray can reveal: Pneumonia or lung infections Fluid around or in the lungs Collapsed lung (pneumothorax) Tumors or masses Enlarged lymph nodes Rib fractures or structural abnormalities Signs of heart enlargement or failure Significant scarring or fibrosis visible on imaging A chest x-ray is quick, widely available, and exposes patients to a small amount of radiation. It is often one of the first imaging tools used when a patient presents with chest pain, shortness of breath, or a suspected infection. According to the National Institutes of Health, chest x-rays are one of the most frequently performed diagnostic imaging studies in medicine, but they have significant limitations when it comes to detecting early or functional lung disease. Pulmonary Function Test vs Chest X-Ray: The Key Differences Understanding how these two tests compare directly is the clearest way to understand when each one is appropriate. Pulmonary Function Test Chest X-Ray Measures Airflow, lung volume, gas exchange Lung and chest structure appearance Detects Asthma, COPD, airflow obstruction Infections, fluid, masses, abnormalities Misses Tumors, infections, fluid, masses Early functional lung disease Radiation None Small dose of ionizing radiation Results Measurements vs predicted normal values Visual findings by a radiologist Best For Diagnosing and monitoring lung function Ruling out structural problems quickly Duration 30 to 60 minutes 10 to 15 minutes Effort Yes – active breathing required No – patient holds still When a Pulmonary Function Test Is the Right Choice A pulmonary function test is typically the better diagnostic tool when: You have symptoms of asthma, COPD, or chronic bronchitis and a diagnosis has not yet been confirmed You are being evaluated for occupational lung disease related to smoke, dust, chemical, or toxin exposure Your provider needs to assess the severity of a known lung condition and track whether it is progressing or improving You are a first responder, firefighter, or worker with regular exposure to airborne hazards You have unexplained shortness of breath during physical activity with no structural findings on imaging Pre-surgical evaluation is needed to assess whether your lungs can handle anesthesia and recovery Monitoring is required for a lung condition being treated with medication For first responders and workers in physically demanding roles, pulmonary function testing provides a functional baseline that imaging cannot. A firefighter may have a normal chest x-ray and still have measurably reduced lung capacity from years of smoke exposure. A PFT catches that where imaging does not. When a Chest X-Ray Is the Right Choice A chest x-ray is typically the better first step when: You have symptoms of pneumonia such as fever, productive cough, and chest pain A lung infection or fluid accumulation is suspected There is concern about a mass, tumor, or enlarged lymph nodes in the chest You have experienced trauma to the chest and rib fractures or pneumothorax need to be ruled out Shortness of breath is sudden in onset and a structural cause needs to be identified quickly Heart enlargement or pulmonary edema is suspected based on symptoms A chest x-ray answers the question of whether something looks abnormal in the chest. A pulmonary function test answers the question of whether the lungs are functioning normally. These are different questions, and both are valid depending on what the clinical