Allergy Testing for First Responders
- Skin Prick Test (SPT): Small amounts of allergens are placed on the skin and lightly pricked to check for quick reactions.
- Blood Test (IgE): A blood sample measures immune response to specific allergens.
- Patch Test:: Patches with allergens are applied to the skin for 48 hours to detect delayed reactions.
- and more!
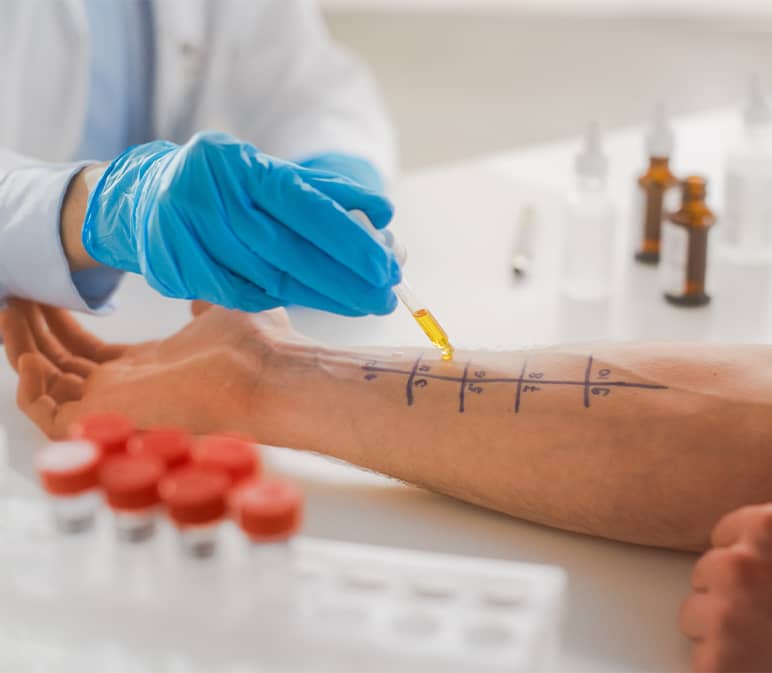
Identifying Triggers That Impact Everyday Health
Why Allergy Testing is Important
Allergies are more than a nuisance. Left unmanaged, they can limit job performance, trigger asthma, and reduce quality of life. Testing helps uncover hidden triggers and provides clear answers to guide prevention and treatment.
First responders often face environments filled with dust, smoke, mold, and other allergens. Left untreated, allergies can:
Compromise breathing during high-stress emergencies
Reduce focus and concentration on the job
Trigger asthma or worsen existing respiratory conditions
Impact energy levels, sleep quality, and overall health
Early testing ensures better prevention, improved treatment, and safer work performance.
Frequent congestion, sneezing, or watery eyes
Chronic cough, wheezing, or shortness of breath
Skin rashes, hives, or unexplained itching
Headaches, fatigue, or brain fog linked to seasonal changes
History of asthma, hay fever, or severe allergic reactions
Occupational exposure to dust, smoke, or chemicals
Early Identification: Detect allergies before they cause long-term complications.
Personalized Care: Tailored strategies to avoid or manage triggers.
Improved Breathing & Performance: Reduced respiratory distress during demanding situations.
Better Sleep & Energy: Relief from chronic congestion and allergy-related fatigue.
Safer Work Environment: Minimize the risk of severe allergic reactions while on duty.
Allergy testing is recommended for:
First responders exposed to environmental hazards daily
Individuals with chronic congestion, cough, or breathing difficulties
Patients with skin reactions such as rashes or hives
Those with a family history of asthma or severe allergies
Anyone experiencing symptoms that worsen during specific seasons or work conditions
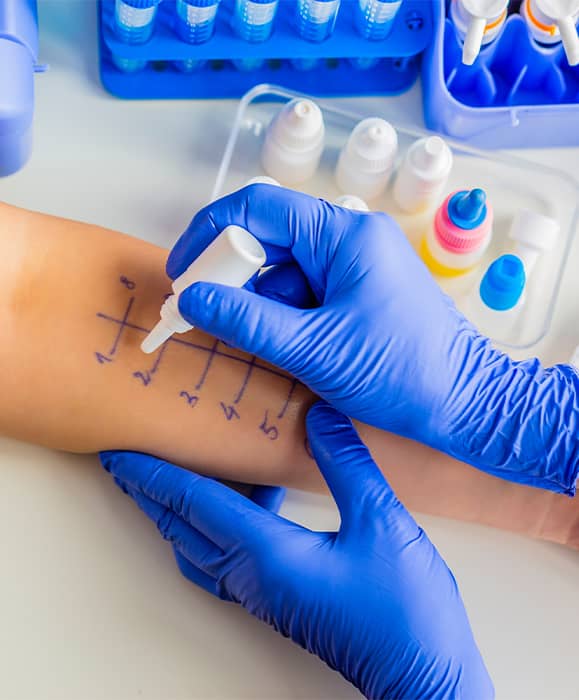
“In 2021, nearly one-third of U.S. adults (31.8%) reported having a seasonal allergy, eczema, or food allergy.” (CDC, 2023)
Frequently Asked Questions
Allergy testing is a medical evaluation that identifies specific substances (allergens) that cause an immune system reaction. This is done through tests such as skin prick testing, blood testing, or patch testing, which measure how your body responds to potential triggers.
Common testing methods include:
Skin prick testing to check for immediate reactions
Blood (IgE) testing to measure immune response to allergens
Pulmonary or breathing assessments to see how allergies impact lung function
First responders are often exposed to smoke, dust, mold, and chemicals that can worsen allergy symptoms. Testing ensures that triggers are identified and managed so symptoms don’t interfere with safety, focus, or performance on duty.
Common signs include frequent nasal congestion, sneezing, itchy or watery eyes, skin rashes, unexplained fatigue, difficulty breathing, or worsening asthma. For first responders, these symptoms may be amplified by occupational exposures.
Patients are typically advised to avoid taking certain antihistamines or medications before testing, as they can interfere with results. Our team will provide clear pre-appointment instructions to ensure accurate testing.
If testing confirms allergies, we provide a personalized treatment plan. This may include avoidance strategies, medication, or referral to specialists for advanced therapies. For first responders, we also recommend workplace adjustments when appropriate.
Yes, allergy testing is safe when performed under medical supervision. Skin reactions are typically mild and temporary. Blood tests carry no additional risk beyond a standard blood draw. Our clinical team monitors all patients closely during testing.
Retesting may be recommended if your symptoms change, if you experience new exposures, or if you begin a different line of work with higher allergen risks. First responders may benefit from periodic re-evaluation due to ongoing occupational exposures.
